Fetal Growth Month by Month: A Complete Trimester-Wise Guide to Physical and Neurological Development
SEO Meta Description: Fetal Growth Month by Month explained in a clear, trimester-wise guide — learn physical and neurological milestones, nutrition tips, monitoring checks, and when to seek care.
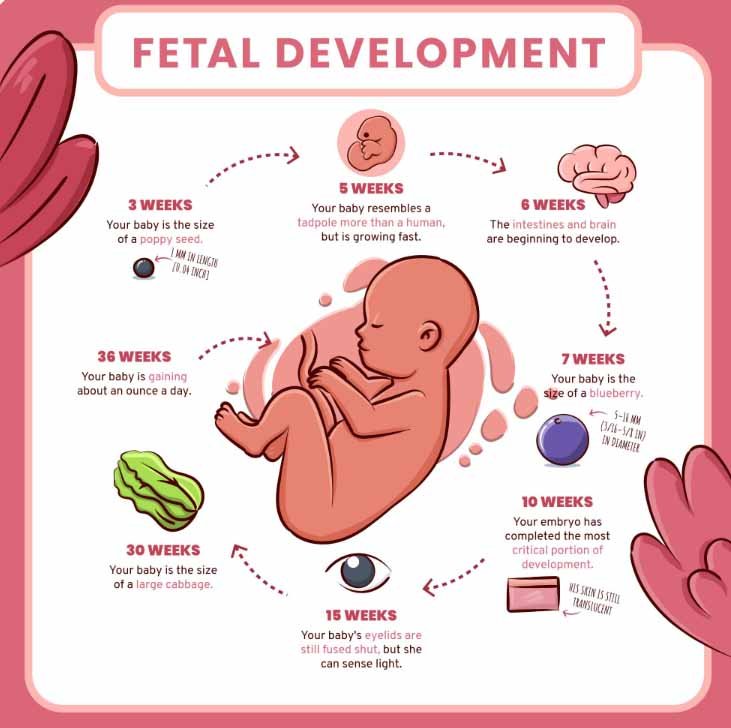
Fetal Growth Month by Month is the roadmap every expecting parent wishes they could see. From the very first cellular divisions to the final weeks of preparation for birth, this guide explains what happens inside the womb and why each stage matters. Understanding these month-by-month changes helps you make healthier choices, reduces anxiety, and deepens the emotional bond with the life growing inside you.
This article is practical and clinician-informed: short, actionable paragraphs, trimester checkpoints, precise guidance about nutrition and tests, and a clear FAQ section so you can use the information immediately.
Why tracking fetal development helps
Following Fetal Growth Month by Month helps parents and clinicians spot milestones and detect concerns early. Regular monitoring builds a timeline of growth, neurological development and organ maturation — allowing timely interventions when necessary.
- ✓ Insight into physical development and organ formation.
- ✓ Understanding neurological milestones and sensory readiness.
- ✓ Guidance for nutrition, activity and prenatal testing to support healthy outcomes.
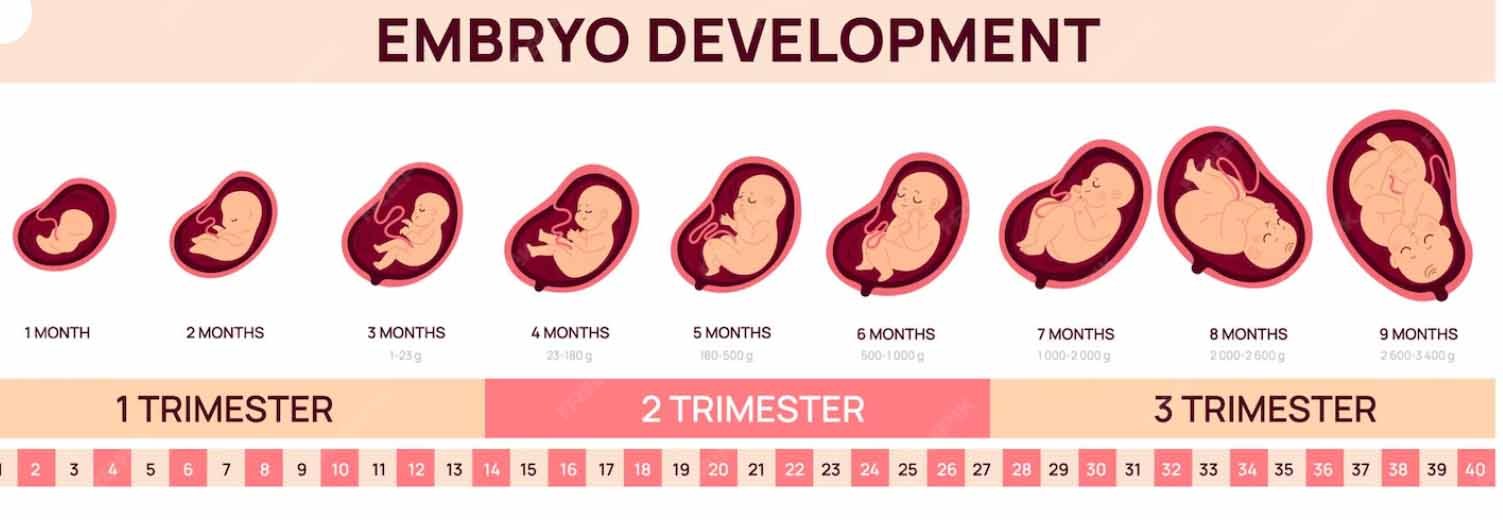
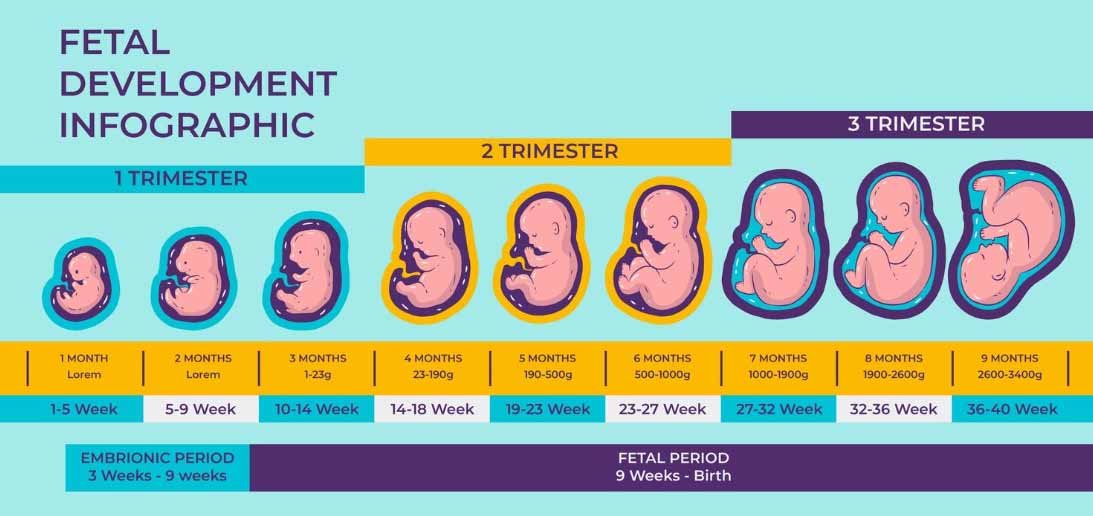
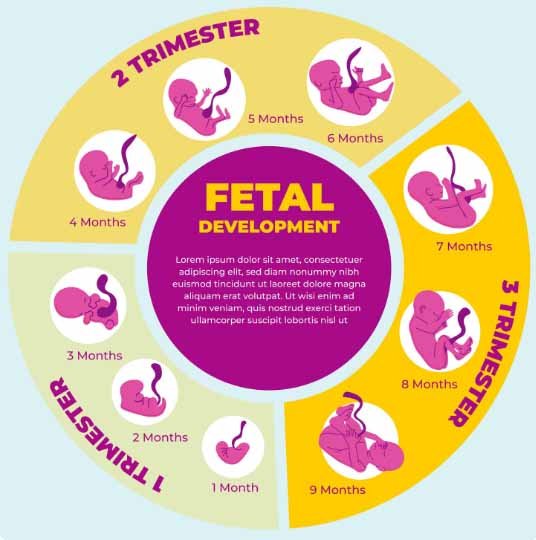
First Trimester (Months 1–3)
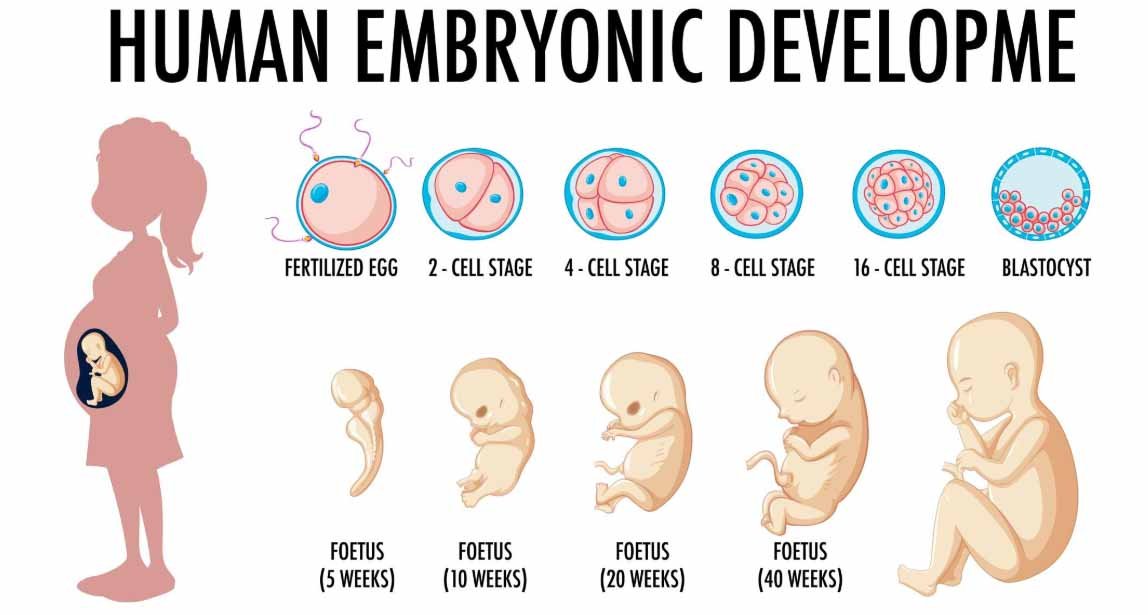
Month 1: Conception and Implantation
Fetal Growth Month by Month begins at fertilization. In month 1, rapid cell division and implantation occur. The embryonic disk forms and the placenta and umbilical structures begin to develop. The neural tube—future brain and spinal cord—starts to close. This period is highly sensitive, so folate intake and avoiding known teratogens matter greatly.
Month 2: Organ Primordia Form
In month 2, early organ buds appear and the heart starts to beat in a regular pattern. Limb buds become rudimentary arms and legs; facial contours begin forming. Because this is the organogenesis window, exposure to alcohol, nicotine and some medications can cause harm.
Month 3: Embryo to Fetus
By the end of month 3 the embryo is now called a fetus. Finger and toe distinction appears, bone ossification begins, and reflexive movements emerge. Most major organ systems are established by now, setting the stage for growth and specialization in later months.
Second Trimester (Months 4–6)
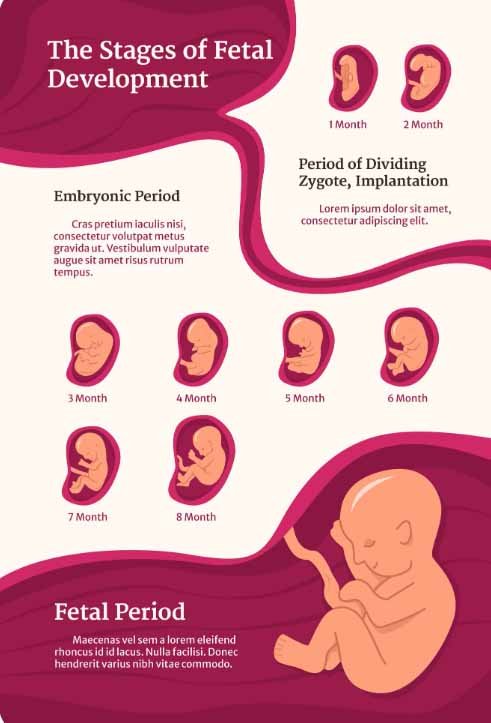
Month 4: Rapid Lengthening and Movement
Growth in month 4 is mostly linear: the fetus gains length, facial features become distinct, and coordinated limb movements strengthen. Parents often begin to notice subtle flutters during this period.
Month 5: Sensory Development
At month 5 the fetus develops lanugo and vernix for protection. Hearing improves and the baby begins to register external sounds. Movements become more pronounced — a major emotional milestone for families following Fetal Growth Month by Month.
Month 6: Brain and Lung Practice
Muscle tone increases, and breathing motions (practice breathing) occur even though lungs are still maturing. The brain forms more complex networks and early sleep cycles begin to appear.
Third Trimester (Months 7–9)
Month 7: Rapid Brain Growth
During month 7 fetal cerebral connectivity expands rapidly and body fat increases to support temperature regulation after birth. Lungs continue to mature and reflexes refine, which improves survival chances for preterm infants born at this stage.
Month 8: Weight Gain and Myelination
Month 8 features rapid weight gain and accelerated myelination — the insulating process that helps neurons transmit signals efficiently. The fetus frequently turns head-down in preparation for labor.
Month 9: Final Maturation
By month 9 organs are mature, reflexes like sucking and grasping are functional, and the baby positions for birth. This month completes the sequence described in Fetal Growth Month by Month as the body and brain prepare for life outside the womb.

Key Nutrients That Support Fetal Growth Month by Month
Throughout pregnancy, certain nutrients play outsized roles:
- ✓ Folate (folic acid): critical in early weeks to prevent neural tube defects.
- ✓ Iron: supports oxygen delivery to the placenta and prevents maternal anemia.
- ✓ DHA (omega-3): supports retinal and brain development.
- ✓ Calcium & Vitamin D: aid skeletal development.
- ✓ Protein: fuels tissue growth across all trimesters.
Balanced meals, hydration, and prenatal supplementation (as recommended by your clinician) provide the best support for consistent growth patterns month by month.
Monitoring, Screening and When to Seek Help
Regular prenatal visits track maternal health and fetal growth using fundal height measurements, Doppler heart checks, and ultrasound scans. Standard scans include:
- ✓ Dating scan in the first trimester.
- ✓ Anatomy (mid-pregnancy) scan around 18–22 weeks.
- ✓ Growth scans later in pregnancy, when clinically indicated.
Seek immediate care for reduced fetal movements, heavy bleeding, severe abdominal pain, sudden swelling, high fever, or persistent headaches with vision changes. Early identification of growth problems or complications allows targeted monitoring and intervention.
Environmental Factors and Medications
Tobacco, alcohol, certain drugs and some prescription medications may impede fetal growth. Occupational exposures, high stress, inadequate sleep and infections can also influence development. Always consult your healthcare provider before starting or stopping medications during pregnancy.
Week-by-Week Highlights (Selected Weeks)
Weeks 1–4: Conception and implantation occur. Early biochemical support builds the placenta and embryonic structures. Folate supplementation is essential.
Weeks 5–8: Organogenesis — the heart begins to beat, limb buds form, and the neural tube closes. This is a high-sensitivity period.
Weeks 9–12: Transition to the fetal period with clearer anatomy and facial formation. First-trimester screenings are commonly offered.
Weeks 13–20: Rapid linear growth, clearer skeletal structures, and early sensory development including hearing.
Weeks 21–28: Continued weight gain, evolving sleep-wake cycles, lung practice movements and the threshold of viability improves in many centers.
Weeks 29–36: Brain growth continues, fat stores accumulate, and positional changes precede labor.
Weeks 37–40+: The baby reaches term readiness; small maturational differences remain among early, full and late term births.
Practical Tips for Supporting Fetal Growth Month by Month
- ✓ Begin prenatal care early and attend scheduled visits.
- ✓ Take prenatal vitamins as advised and prioritize nutrient-dense foods.
- ✓ Engage in gentle regular activity like walking or prenatal yoga.
- ✓ Avoid smoking, alcohol, and unnecessary medications without clinician approval.
- ✓ Practice stress management and ensure adequate sleep to support maternal and fetal wellbeing.
- ✓ Monitor fetal movements in the third trimester and report any sustained decreases.
When to Contact Your Healthcare Provider
- ✓ Reduced or absent fetal movements compared with usual patterns.
- ✓ Severe abdominal pain, heavy vaginal bleeding, or leaking fluid.
- ✓ High fever, severe headache, visual disturbances or sudden pronounced swelling.
Frequently Asked Questions
Q1: What are the main stages of fetal growth month by month?
A1: Broadly: the first trimester establishes organs and structures, the second trimester expands growth, movement and sensory development, and the third trimester completes maturation and readies the baby for birth.
Q2: When will I feel my baby move?
A2: Many parents feel first movements between 16–22 weeks. First-time parents may notice later than those with previous pregnancies.
Q3: How does the fetal brain develop in the womb?
A3: Neural tube formation begins early; neuron proliferation and network formation accelerate in mid-pregnancy; late pregnancy massively increases synapse formation and myelination.
Q4: What affects birth weight?
A4: Genetics, maternal nutrition and health, placental function, and environmental exposures are major contributors to birth weight.
Q5: When is pregnancy full term?
A5: Full term is generally 39–40 weeks. Term ranges include early term (37–38 weeks), full term (39–40 weeks), late term (41 weeks) and post-term (42+ weeks).
Further Reading & Resources
Trusted resources include national obstetrics guidelines, local prenatal clinics and peer-reviewed articles about prenatal development. Speak with your clinician for individualized recommendations and for resources tailored to your health history.
Join our prenatal resources
Sign up for printable month-by-month checklists, meal plans, and short guides to help you follow Fetal Growth Month by Month with confidence.
- ✓ Weekly milestone checklists
- ✓ Nutrient-focused meal suggestions
Conclusion
Fetal Growth Month by Month offers a structured way to appreciate fetal development from conception to birth. While genetics and biology drive much of development, maternal nutrition, prenatal care and healthy behaviors support the best possible outcomes. Celebrate the milestones, ask questions at appointments, and prepare for birth with evidence-based choices.
If you have pregnancy-specific medical conditions (gestational diabetes, hypertension, etc.), partner with your provider to personalize care. Most pregnancies proceed well when guided by attentive prenatal care and supportive lifestyles.